The State of Male Fertility: A Declining Trend
The successful creation of a baby requires three main ingredients:
- A healthy egg (female)
- Healthy sperm (male)
- A receptive uterus (“belly”) to grow
Although it takes two people to conceive, women often shoulder most of the attention and burden in fertility and conception, especially when it isn’t working. This bias is problematic. Male fertility is often treated as a secondary issue, yet up to 40–50% of infertility cases involve a male factor 10, 12. With men contributing equally to fertility outcomes, it’s only fair, and necessary, to pay equal attention to sperm health.
In this post we’ll review recent trends in male fertility, what the data suggests about broader health implications, and next steps you can take to evaluate male fertility and overall well‑being.
The Data Sperm Counts are Falling
Multiple large-scale studies and systematic reviews show a marked decline in sperm concentration (SC) and total sperm count (TSC) over the past several decades across the globe, especially in higher-income countries 6, 10, 11, 12, 16. Other sperm quality parameters including progressive motile sperm (PR) have also shown a downward trend, while the total motile sperm (TM) trend has not yet reflected a downward or even leveling off trajectory 12.
Meta-analyses dating back to the 1970s report declines in sperm concentration of roughly 50% or more in many regions 10, 11, 12. The data is also revealing other patterns:
- The rate of sperm count decline is accelerating!
- Between 1973-2000, sperm count fell by ~1.16% per year 10, 11
- After 2000, the rate of decline has fallen faster to about 2.64% per year 10, 11
- The male infertility burden is increasing!
- Between 1990 and 2019, the global occurrence of male infertility increased by 76.9% 7. The highest burden is being seen in South Asia (India, China, Indonesia).
- Regional variations are linked to other factors beyond genetics! 6, 10, 11
- Environmental exposures, lifestyle factors and pollution have been linked to the declining sperm count trend seen around the globe.
- Sperm count projections into the future look bleak!!
- If left unchecked, extrapolating the 2017 meta-analysis trend line projects that the median male sperm count could approach zero by 2045 18.
- Testosterone levels are also dropping!
- A global analysis by Santi et al. (2025) showed “a significant decrease in mean total testosterone serum levels in over one million healthy men over the last 55 years” and what’s more is that this “declining trend is associated with a significant decrease in LH serum levels, indicating that the testosterone decline does not primarily originate in the testis.” 16
- (P.S. There is a well documented relationship between obesity and testosterone serum levels. Keep reading below!)
To view a visual representation of the male fertility trends occurring across the globe, check out Figure 1: Male infertility and assisted reproduction globally from this article by Nosrati, et al. (2017)15.
Concurrent Health Trends
While sperm count has declined globally, other health conditions have also risen in parallel with nearly every country following the same trajectory. Specifically, on a global scale:
- Obesity rates have roughly tripled in many populations indicating that over 1 in 8 adults now live with obesity 19
- Type 2 diabetes has increased 5x 14
- Metabolic syndrome has increased several fold over recent decades, especially in regions where obesity and type 2 diabetes are rising quickly 13
- Autoimmune disorders have steadily increased over the last 3 decades 20
- Testicular Cancer up 28% 3
These trends are not independent of each other. And more importantly, they are NOT coincidental! There are shared risk factors and biology that connects sperm health to health in the rest of the body systems. Sperm health is the reflection of the greater underlying health status in the body.
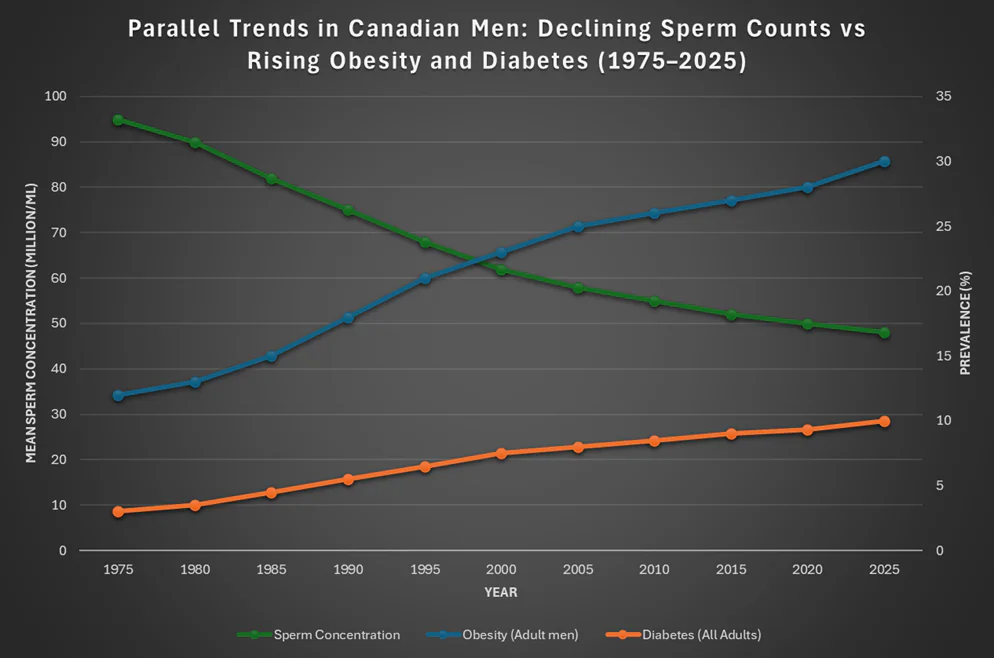
Trends adapted from Younglai (1998) 21, Statistics Canada CCHS 17, Diabetes Canada CPG 4
Sperm Count & Future Health Outcomes
Recent literature is now starting to acknowledge that low sperm count is more than just a fertility issue…it is a biomarker of broader health risks! 2, 3, 5, 8, 9
There is shared physiological pathways between male infertility and development of chronic diseases including inflammation, oxidative stress, immune and hormonal dysfunction.
A systematic review of multiple cohort studies found associations between male infertility and many chronic diseases. Men diagnosed with infertility had higher risks of developing in the future:
- Cardiovascular (heart) disease
- Hazard ratios* in several studies range roughly 1.2–1.6 5, 9
- Metabolic syndrome (also called insulin resistance syndrome; is at least 3 or more of the following conditions: abdominal obesity, high blood pressure, high blood sugar levels, high blood triglycerides, low HDL cholesterol)
- Odds ratios* ~1.5–2.0 2, 12
- Type 2 Diabetes
- Hazard ratios around 1.4 5
- Hypogonadism (the body makes too little testosterone or the testes don’t work properly)
- Substantially higher odds for men with low sperm counts (for example, OR ≈ 12 in some analyses for very low counts)16
- Increased all-cause morbidity and earlier mortality in some cohorts 2, 5, 8, 9
- Increased risk incidence of testicular and prostate cancer 2,3

Why This Matters- Beyond Conception
There are considerable implications behind all these stats. On an individual level, these stats reflect a detrimental impact to all domains of health and well-being:
- Physical impactà Compromised current and future health & longevity
- Mental Health à Spiraling and dysfunctional thoughts
- Emotion Health à Hard emotions like shame, guilt, hopelessness, despair
- Spiritual Health à Lost meaning and purpose in life (lost dreams of fatherhood, impact of childlessness)
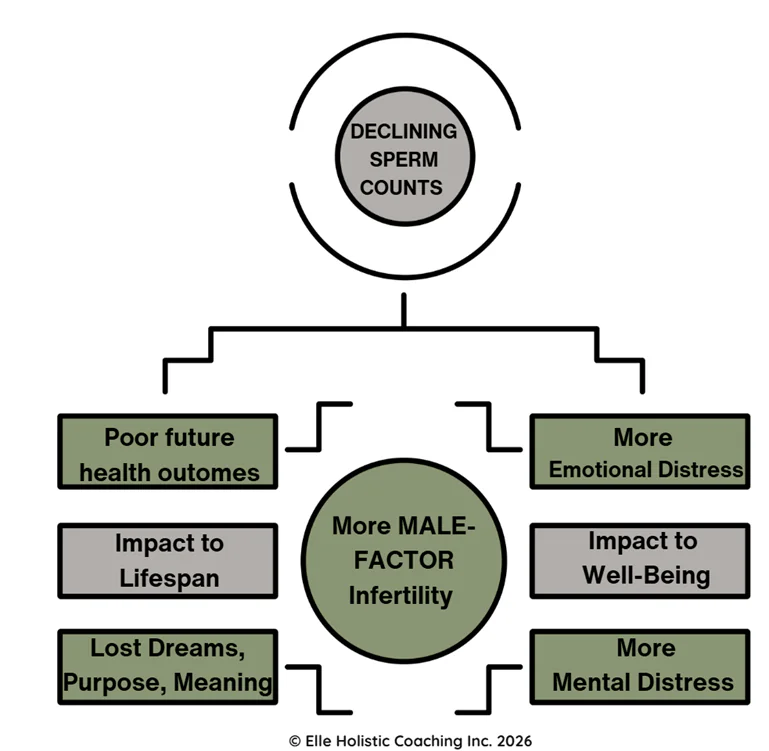
Addressing sperm health therefore has benefits beyond fertility: it can be a window into your long-term health and an opportunity to intervene early.
Overlooked Contributors
Now that we understand the connection between sperm health and overall health, the next step is to explore the underlying factors contributing to these two health trajectories.
Modern life is exposing men to numerous modifiable risk factors that are impairing sperm quality. High-quality studies (systematic reviews, meta-analyses, and large cohorts) have validated this connection to lifestyle factors. Specifically, that poor diet, sedentary behavior, stress, toxins, smoking and alcohol among other lifestyle factors are associated with poor semen quality and infertility1.
The good news is that many of these factors are within one’s control and can be improved!
What You Can Do Next
Your first thought is probably: “I need to get my sperm count checked.”
A semen analysis is a valuable starting point for evaluating male fertility, but it’s only one part of the puzzle. Revealing the root causes behind poor results is even more crucial. Understanding your individual risk factors that could be affecting the quality of your sperm is essential for taking meaningful action towards improvement.
Finding a provider who first acknowledges this connection between overall health and sperm health while understanding the deeper implications is critical.
Additionally, working with a provider who takes a holistic approach by assessing lifestyle, metabolic status, hormonal function, environmental exposures, sleep and stress patterns, as well as emotional and mental health, can be one of the best steps you can take. This approach will help you identify root causes affecting your fertility and provide a personalized plan to move forward in improving both fertility and long‑term health.
Want an evaluation of your health & fertility?
Book a Free 60-minute Discovery Call and we’ll review your top concerns, and determine the next best steps to get you the information you deserve.
Want to learn more?
Join my mailing list / newsletter: Subscribe for practical tips, and evidence-based insights that show how to address root causes rather than just silence symptoms.
References
1 Balawender, K., & Skrzypulec-Plinta, V. (2020). The impact of selected modifiable lifestyle factors on male fertility in the modern world. Central European Journal of Urology, 73(4):563–568 https://pmc.ncbi.nlm.nih.gov/articles/PMC7848840/
2 Del Giudice, F., et al. (2020). Clinical correlation among male infertility and overall male health: A systematic review of the literature. Investigative and Clinical Urology, 61 (4): 355–371. doi: 10.4111/icu.2020.61.4.355
3 Del Giudice, F., et al. (2020). Association between male infertility and male-specific malignancies: systematic review and meta-analysis of population-based retrospective cohort studies. Fertility & Sterility, 114(5):984-996. https://pubmed.ncbi.nlm.nih.gov/32709378
4 Diabetes Canada Clinical Practice Guidelines Expert Committee. (2018). Diabetes Canada 2018 clinical practice guidelines for the prevention and management of diabetes in Canada. Canadian Journal of Diabetes, 42(Suppl 1), S1–S325. https://pmc.ncbi.nlm.nih.gov/articles/PMC6347316/
5 Eisenberg, M.L., et al. (2016). Increased risk of incident chronic medical conditions in infertile men: analysis of United States claims data. Fertility & Sterility, 105(3), 629-36. http://dx.doi.org/10.1016/j.fertnstert.2015.11.011
6 Feferkorn, I., et al. (2022). Geographic variation in semen parameters from data used for the World Health Organization semen analysis reference ranges. Fertility & Sterility, 118(3), 475-82. https://doi.org/10.1016/j.fertnstert.2022.05.037
7 Huang, B., et al. (2023). Global, regional and national burden of male infertility in 204 countries and territories between 1990 and 2019: an analysis of global burden of disease study. BMC Public Health, 23(1): 2195. https://pmc.ncbi.nlm.nih.gov/articles/PMC10631182/
8 Kaltsas, A., et al. (2025). Male Infertility and Reduced Life Expectancy: Epidemiology, Mechanisms, and Clinical Implications. Journal of Clinical Medicine, 14(11):3930. https://pmc.ncbi.nlm.nih.gov/articles/PMC12156384/
9 Latif, T. et al. (2017). Semen Quality as a Predictor of Subsequent Morbidity: A Danish Cohort Study of 4,712 Men With Long-Term Follow-up. 186 (8): 910-917. doi: 10.1093/aje/kwx067
10 Levine, H., et al. (2023). Temporal trends in sperm count: a systematic review and meta-regression analysis of samples collected globally in the 20th and 21st centuries. Human Reproduction Update, 29 (2): 157-176. doi: 10.1093/humupd/dmac035
11 Levine, H., et al. (2017). Temporal trends in sperm count: a systematic review and meta-regression analysis. Human Reproduction Update, 23 (6): 646–659. doi: 10.1093/humupd/dmx022
12 Luo , X., et al. (2023). Global trends in semen quality of young men: a systematic review and regression analysis. Journal of Assisted Reproduction and Genetics, 40(8):1807–1816. https://pmc.ncbi.nlm.nih.gov/articles/PMC10371917/
13 National Heart, Lung and Blood Institute (NHLBI). (2022). What is metabolic syndrome? https://www.nhlbi.nih.gov/health/metabolic-syndrome#
14 NCD Risk Factor Collaboration (NCD-RisC). (2024). Worldwide trends in underweight and obesity from 1990 to 2022: a pooled analysis of 3663 population representative studies with 222 million children, adolescents, and adults. Lancet, 403: 1027-50. https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(23)02750-2/fulltext
15 Nosarati, R., et al. (2017). Microfluidics for sperm analysis and selection. Nature Reviews Urology, 14, 707-30. https://www.nature.com/articles/nrurol.2017.175#Abs1
16 Santi, D., et al. (2025). Temporal trends in serum testosterone and luteinizing hormone levels indicate an ongoing resetting of hypothalamic-pituitary-gonadal function in healthy men: a systematic review. Journal of Endocrinological Investigation, 48, pages 2721–2734. https://link.springer.com/article/10.1007/s40618-025-02671-9
17 Statistics Canada. (2023). Canadian Community Health Survey (CCHS) – Obesity prevalence trends. https://www.canada.ca/en/public-health/services/publications/healthy-living/obesity-statistics-canada.html
18 Swan, S. (2021). Interview and commentary on projected sperm count trends. Environmental Health News. https://www.ehn.org/fertility-crisis
19 World Health Organization (WHO). 2025). Fact Sheet: Obesity and overweight. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
20 Xiao, X-P., et al. (2026). Global landscape of autoimmune diseases across different lifespan: A three-decade perspective. Medicine; 105(2):e47140. doi: 10.1097/MD.0000000000047140
21 Younglai, E. V., Collins, J. A., & Foster, W. G. (1998). Canadian semen quality: An analysis of sperm density among eleven academic fertility centers. Fertility and Sterility, 70(6), 1051–1056. https://pubmed.ncbi.nlm.nih.gov/9660425/